
Fasting has become one of the most popular strategies for improving metabolic health, supporting weight loss, and enhancing cellular repair. From intermittent fasting to multi-day water fasts, millions of people are experimenting with different fasting protocols.
But there is one factor that often gets overlooked - electrolytes.
Many people assume that fatigue, headaches, or dizziness during fasting are simply part of the "detox process." In reality, those symptoms are frequently related to electrolyte imbalance.
Understanding how electrolytes function during fasting can make the difference between a smooth fast and a miserable one. As a registered nurse, I've seen firsthand how important electrolyte balance is for maintaining energy, hydration, and neurological stability.
This guide explains what electrolytes are, why they become depleted during fasting, and how to maintain proper electrolyte levels so your body can adapt safely.
What Electrolytes Are and Why They Matter
Electrolytes are minerals that carry an electrical charge when dissolved in water. These minerals help regulate critical functions throughout the body, including:
- nerve signaling
- muscle contraction
- hydration balance
- blood pressure regulation
- heart rhythm
The most important electrolytes for fasting include:
- sodium
- potassium
- magnesium
These minerals allow cells to communicate with each other and maintain proper fluid balance between the inside and outside of cells.
Even small changes in electrolyte levels can lead to noticeable symptoms such as fatigue, muscle cramps, or headaches.
Why Fasting Depletes Electrolytes
When you stop eating, your body begins transitioning from using glucose as its primary fuel source to burning stored fat.

During the early stages of fasting, insulin levels drop. This shift triggers the kidneys to release excess sodium and water through urine. As sodium is excreted, other electrolytes like potassium and magnesium may also be lost.
Several factors contribute to electrolyte depletion during fasting:
Increased urination
Lower insulin levels signal the kidneys to excrete sodium. This causes a temporary loss of both salt and water.
Reduced dietary intake
When food intake stops, dietary sources of minerals disappear as well.
Glycogen depletion
Stored glycogen binds water and electrolytes. As glycogen is depleted, additional water and minerals are released.
These combined factors can lead to symptoms if electrolytes are not replenished.
Symptoms of Electrolyte Imbalance During Fasting
Many of the unpleasant symptoms associated with fasting are actually related to electrolyte loss rather than the absence of calories.
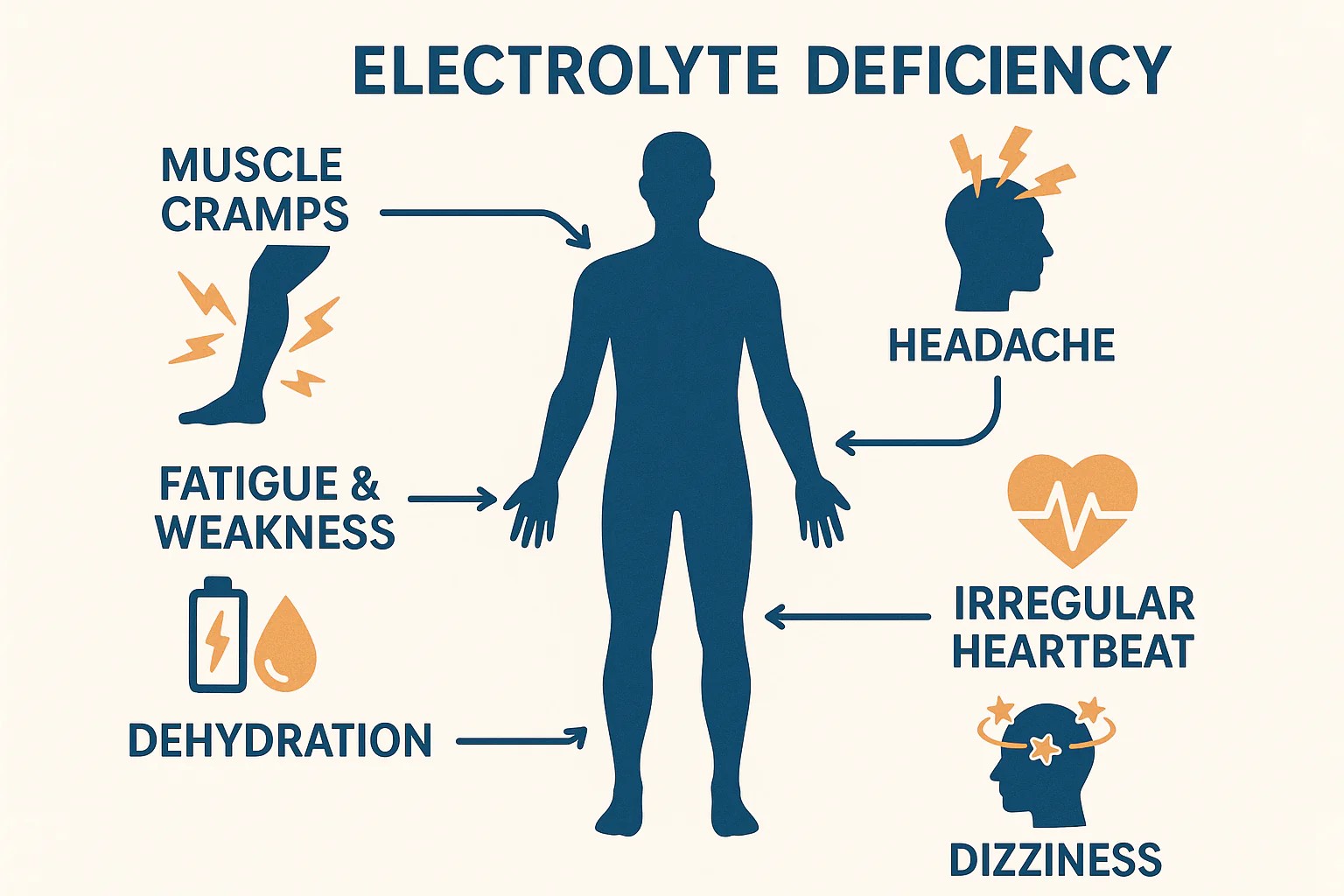
Common symptoms include:
- headaches
- dizziness or lightheadedness
- fatigue
- muscle cramps
- brain fog
- nausea
- weakness
- heart palpitations
From a clinical perspective, sodium depletion is often the most common issue during extended fasting. When sodium levels drop, blood volume can decrease slightly, which may contribute to headaches and fatigue.
While mild symptoms are common during early fasting adaptation, persistent or severe symptoms should not be ignored.
The Three Key Electrolytes You Need While Fasting
Maintaining proper levels of sodium, potassium, and magnesium can significantly improve the fasting experience.
Sodium
Sodium is the most critical electrolyte during fasting.
It helps regulate:
- fluid balance
- nerve transmission
- blood pressure
When insulin levels drop during fasting, the kidneys release sodium through urine. Without replacement, this loss can contribute to fatigue and headaches.
Adding sodium back into the body is often the fastest way to relieve fasting-related symptoms.
Potassium
Potassium works closely with sodium to regulate cellular fluid balance and nerve signaling.
It plays an important role in:
- muscle contraction
- heart rhythm
- nerve communication
While potassium losses during fasting are usually smaller than sodium losses, maintaining adequate potassium intake supports overall electrolyte balance.
Magnesium
Magnesium is involved in hundreds of biochemical reactions within the body.
It supports:
- muscle relaxation
- nerve function
- sleep quality
- energy production
Low magnesium levels can contribute to muscle cramps, fatigue, and poor sleep during fasting.
These two supplements are my favorite forms of magnesium: Magnesium Glycinate and Calm Powder
Why Fasting Headaches Happen
Headaches are one of the most common complaints during the first 24-72 hours of fasting.
Several factors can contribute to fasting headaches:

Electrolyte depletion
Low sodium levels may reduce circulating blood volume, contributing to headache symptoms. In clinical settings, low sodium can present as headaches, fatigue, and confusion. People attempting extended fasting often mistake these symptoms for 'detox' when they may actually indicate electrolyte imbalance.
Dehydration
Increased water loss through urine can lead to mild dehydration if fluid intake is not increased.
Caffeine withdrawal
People who regularly consume coffee or caffeine may experience withdrawal headaches when fasting.
Blood sugar fluctuations
The body may need time to adapt to burning fat and ketones instead of glucose.
In many cases, adding sodium and increasing hydration significantly reduces fasting headaches.
How Much Sodium, Potassium, and Magnesium You Need
Electrolyte needs vary depending on the individual, the length of the fast, activity levels, and climate.
However, general guidelines during extended fasting may include:
Sodium
Approximately 2,000-2,300 mg per day
This is often the most important electrolyte to replenish.
Potassium
Approximately 2600 mg for women (age 19+) and 3400 mg for men (age 19+)
Potassium helps maintain fluid balance and nerve function.
Magnesium
Approximately 300-400 mg per day
Magnesium supports muscle relaxation and sleep quality.
These values are general estimates and may not be appropriate for everyone. Individuals with certain medical conditions, including kidney disease or heart conditions, should consult a healthcare professional before attempting extended fasting.
Best Electrolyte Drinks During Fasting
Electrolyte drinks can help replenish minerals while keeping calorie intake minimal.
Here are some common options: 9 Drinks You Can Have Without Breaking Your Fast

Overall, when choosing an electrolyte drink during fasting, it is important to avoid beverages that contain large amounts of sugar or calories if the goal is to maintain a fasted state.
Homemade Electrolyte Drink Recipe
A simple homemade electrolyte drink can provide essential minerals while avoiding artificial ingredients.
See the recipe here: Homemade Electrolyte Drink for Extended Fasting

This simple mixture helps replenish sodium and potassium while supporting hydration.
Many people find that adding electrolytes significantly improves their energy levels and reduces headaches during fasting.
When Fasting Becomes Unsafe
While fasting can offer metabolic benefits, it is not appropriate for everyone.
Certain individuals should avoid extended fasting or only fast under medical supervision.
These groups may include:
- individuals with diabetes requiring medication
- people with kidney disease
- pregnant or breastfeeding women
- individuals with a history of eating disorders
- those taking medications affected by food intake
Symptoms such as severe dizziness, confusion, fainting, or irregular heartbeat should always be taken seriously and evaluated by a healthcare professional.
Fasting should support health - not compromise it.
FAQs About Electrolytes and Fasting
Electrolytes themselves do not contain calories and generally do not break a fast. However, some electrolyte drinks contain sugar or artificial sweeteners that may affect metabolic responses.
Headaches during fasting are often related to sodium depletion, dehydration, caffeine withdrawal, or temporary metabolic adjustments.
Symptoms such as fatigue, dizziness, muscle cramps, and headaches can indicate electrolyte imbalance. Persistent symptoms should be evaluated by a healthcare professional.
Because fasting causes the kidneys to excrete more minerals, sodium becomes the most essential electrolyte to replenish. Maintaining sodium levels is vital for controlling blood pressure and preventing ‘fasting flu’ symptoms like fatigue and headaches. It also acts as the primary driver for hydration, ensuring water is absorbed by your cells rather than flushed out.
Yes. Many people use electrolytes during intermittent fasting to maintain hydration and reduce symptoms such as fatigue or headaches. You can make your own electrolyte mix for fasting or you can purchase LMNT which comes in several different flavors.
Sure, you can have bone broth while fasting, but you technically won’t be in a “fasted” state anymore; this would be more along the lines of “liquid fasting”. Sipping bone broth will kick you out of a fasted state because the amino acids and collagen stimulate insulin, halting the metabolic rest achieved during a true fast.
This would be more along the lines of “liquid fasting”. Drinking protein shakes will kick you out of a fasted state because they contain calories, macronutrients, and added flavorings stimulating insulin, halting the metabolic rest achieved during a true fast.
Electrolytes play a critical role in maintaining balance during fasting. When insulin levels drop and the body begins excreting sodium and water, electrolyte levels can shift quickly.
Understanding how to replenish sodium, potassium, and magnesium can help prevent many of the symptoms commonly associated with fasting, including headaches, fatigue, and muscle cramps.
Fasting should feel manageable and sustainable. Supporting your body with proper hydration and electrolyte balance can make the experience far more comfortable while allowing you to focus on the metabolic benefits that fasting provides.
More articles on fasting:
10 Intermittent Fasting Tips You Should NOT Follow
What Happens to your Body During a Water Fast




Chime in--Join the Discussion!